Drug overdoses have taken a heavy toll on British Columbians over the last year and have not left the Lakes District unscathed.
For September, the last month that data was made available, 128 people province-wide died of illicit drug overdoses, and 1,143 died in 2018, according to data from the BC Coroners Service.
READ MORE: B.C. on track to record same number of overdose deaths as last year
In the northern B.C. context, deaths from illicit drug overdoses have increased each year since 2009, and 60 people died this year until September.
Prince George was the seventh highest township (out of 16) in the province for deaths by overdose in 2018, with 30 deaths.
Many drug overdoses involve opioid painkillers like the particularly powerful and dangerous drug fentanyl.
RELATED: Interlakes mom mourns son after fentanyl overdose
Unlike the Coroners Service report, which covers overdoses of all drugs, Northern Health has compiled data specifically on opioid overdoses in northern B.C.
In its “Public ED Enhanced Surveillance” report released in September, the service tracked opioid overdose incidents that resulted in visits to emergency departments (EDs), such as hospital emergency rooms.
The report focussed on the period since June 13, 2016 and was concerned only with the 1,135 overdoses in that time.
The overdoses did not necessarily cause death.
In the north there have been an average of 10 overdose-related emergency department visits per week since January 2017.
Almost 30 visits happened in one week at the end of July of last year.
In an overview of the northern region from Prince George to Prince Rupert, less than 15 emergency visits in Burns Lake were noted in the last two years, and less than five this year.
Burns Lake had the least amount of visits of all the towns in this area including Vanderhoof, Fort St.James, Smithers and Hazelton.
Prince George, on the other hand, with its much higher population had hundreds of emergency visits in that period.
Despite the lower population of the Lakes District and the apparently less severe state of drug use compared to other parts of the province, health authorities here are still prepared.
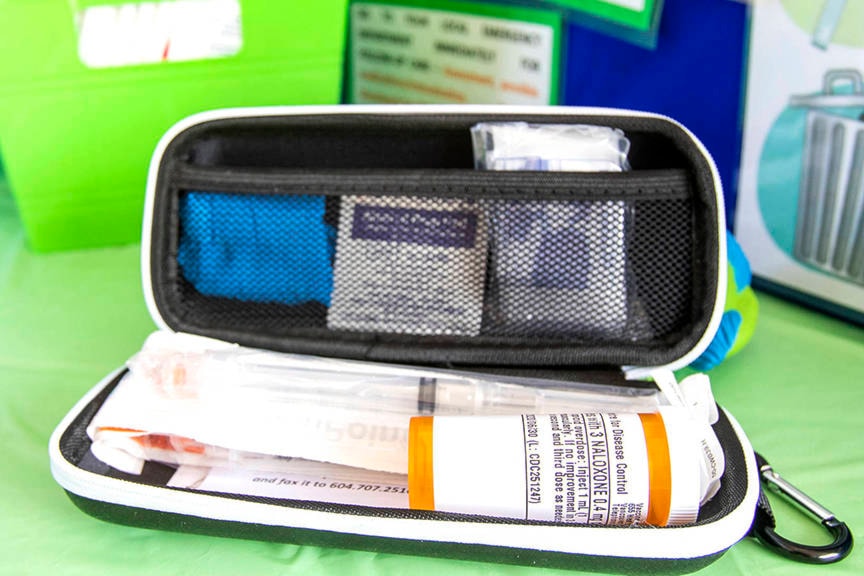
Dozens of kits containing Naloxone, a medication that reverses the effects of opioid overdoses, have been distributed to local healthcare providers such as the hospital in Burns Lake and the Grand Isle and Southside Health Centres.
“[The kits are] handed out there and there’s a supply there. They’re also easy to order,” Marie Hunter, Health Services Administrator with Northern Health told Lakes District News.
“All the staff who deal with the public have been trained in harm reduction,” she said.
The Southside Health & Wellness Centre currently has about 15 naloxone kits on hand and has had them available since late 2016, said the centre’s manager Aileen Serle.
A Burns Lake health care worker said there has been moderate interest in the naloxone kits.
“Sometimes it’s just family members coming in because they think someone has a problem,” the worker said.
“Sometimes in a small community they don’t want to admit that they need them. As far as confidentiality it’s hard in a small community because we all know each other.”