Rural residents in B.C. have to pay extra costs for healthcare, travel longer distances than their urban peers, and go through additional stress as a result.
These were the findings of a survey led by Dr. Jude Kornelsen for BMC Health Services Research and distributed by the BC Rural Health Network (BCRHN), an organization recently joined by the Village of Burns Lake and has Fraser Lake’s Bob Storey as a board director.
While it’s true that Canada’s healthcare system spares an individual from having to pay for a lot of up-front expenses and gives equal access regardless of who is at the door of need, there are many expenses patients must pay out of pocket while getting to the door, and for services that are not covered by the program [physiotherapy, prescription drugs, post-surgical materials, etc.]. These areas were of particular interest to Kornelsen and the BCRHN.
“The cost of seeking health care is a significant burden for many rural residents in British Columbia,” said BCRHN executive director Paul Adams. “The survey found that nearly 80 per cent of rural respondents had difficulty paying for their care, and 60 per cent reported that travelling to access care negatively affected their health.”
Adams said that particularly rural factors also made things worse, like “a lack of public transportation options, (and) unfilled positions in community health facilities…As a result, many residents are forced to delay or diminish their care-seeking, leading to negative impacts on both their health and the overall healthcare system.”
Adding to the payments the patient so often must make, rural sufferers often have to have someone accompany them, which adds costs. There is also an inordinate amount of lost wages, childcare, house-sitting and other bills beyond direct medical items because of the longer lengths of time a rural patient must be away from work compared to an urban resident.
It is hard to calculate the cost of anxiety, but these patients all too often report stress linked to these extra expenses.
“Many participants expressed that having to travel for certain types of care was expected as a rural resident. However, they also felt that there were some essential services that should be available in their local community but were lacking,” Kornelsen said. “Most notably, there was a perception that many rural communities are lacking an adequate number of family doctors, leading to an over- reliance on emergency services. As a result of the closure of the walk-in clinic in their rural community, one participant even commented that they felt they had no other choice but to pay for private care.
“A second rural health gap described by some respondents was the lack of alternatives to in-person specialist visits, such as visiting specialists or opportunities for virtual care. This was perceived by some participants to be the result of inadequate systems planning.”
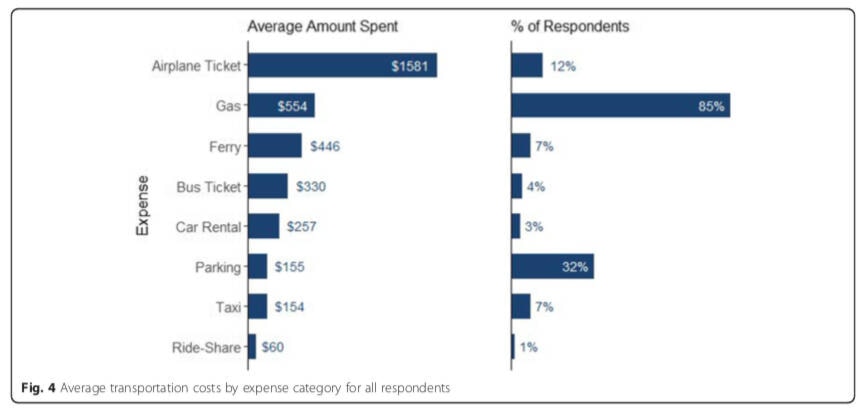
The research reflected an estimated average cost of $2,044 per condition, for rural patients.
“Providing better access to care and removing financial barriers is essential for improving the health and wellbeing of our rural residents,” said Paul Adams, Executive Director of the BC Rural Health Network. “The BC Rural Health Network is committed to working with the government to address these challenges and improve access to care for rural residents.”
Numbers of respondents per community were not disclosed on an individual level, but research did indicate the general Lakes District area had about 50 who contributed to the data.